Artificial Intelligence Monitoring of Neurological Status From Patient Videos in the Neuroscience Intensive Care Unit
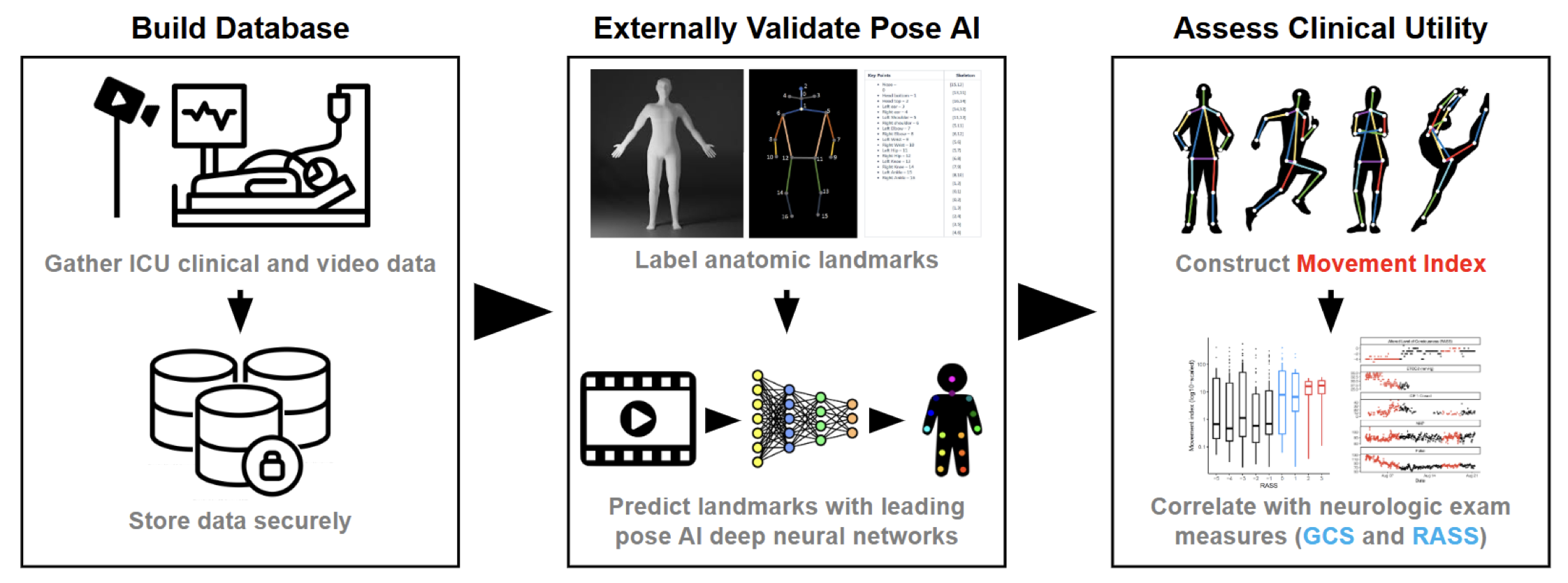
In this study, we evaluated the feasibility of artificial intelligence (AI)-based pose estimation as a method for continuous neurological monitoring in the neuroscience intensive care unit (NSICU). Traditional neurological examinations, while essential, are intermittent, examiner-dependent, and often unavailable in hospitals without subspecialized neurocritical care services. We retrospectively analyzed 998,520 minutes of video-electroencephalography recordings from 119 NSICU patients and externally validated two leading pose estimation models, identifying ViTPose as the superior performer. Using this model, we developed a novel computer vision-derived movement index (λMI) that demonstrated strong, graded correlations with established measures of consciousness, including the Glasgow Coma Scale (GCS) and the Richmond Agitation Sedation Scale (RASS). Movement increased 21-fold across GCS strata and 10-fold between sedated and awake/agitated states, consistent with clinical expectations. These findings support AI-based pose estimation as a minimally invasive, scalable, and clinically meaningful approach to continuous neuromonitoring in critically ill patients.
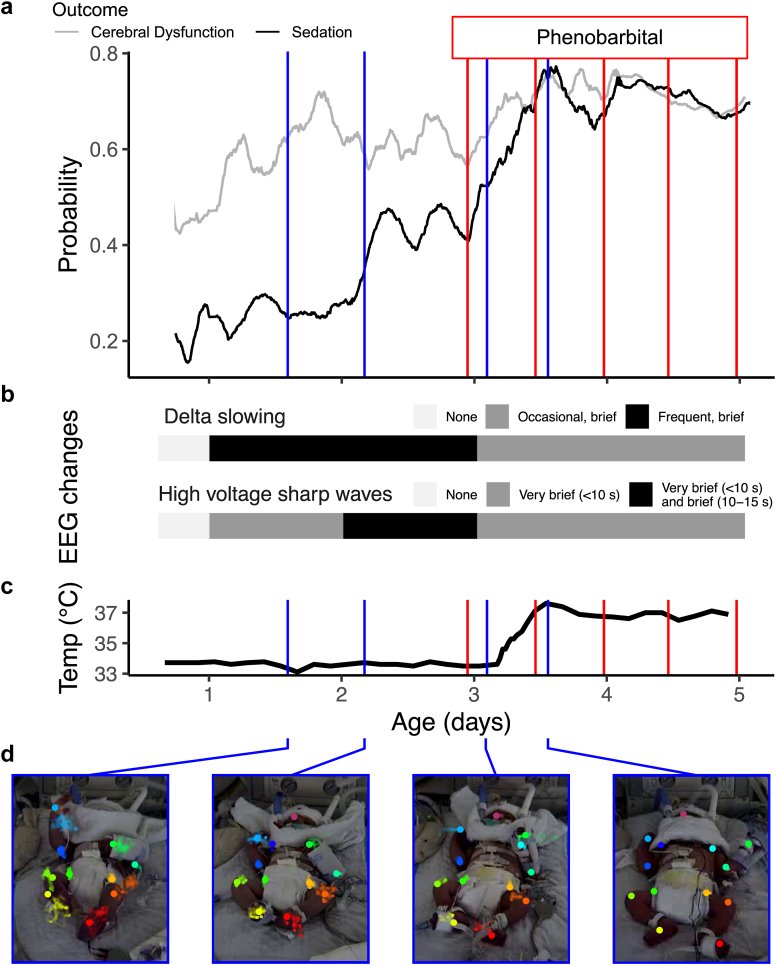
In this study, we investigated whether artificial intelligence (AI)-based pose estimation could enable continuous, objective neurological monitoring in the neonatal intensive care unit (NICU). We assembled the largest video-electroencephalography (video-EEG) dataset to date, comprising 282,301 minutes of video from 115 infants, and trained a deep learning model to identify 14 anatomical landmarks from bedside video feeds. Using these pose-derived features, we developed classifiers to predict sedation exposure and cerebral dysfunction, as determined by EEG interpretation from an epileptologist. The model demonstrated strong performance across cross-validation, held-out frames, and held-out infants, with ROC-AUCs up to 0.91 for both sedation and cerebral dysfunction. After adjusting for age, reduced movement was significantly associated with sedative administration and EEG-confirmed cerebral dysfunction. These findings support pose-based computer vision as a scalable, minimally invasive approach to neuro-telemetry and early detection of neurological impairment in critically ill infants.